 The specifics of these features will be described for both percutaneous and paddle-type leads. The proximal portion of the paddle is typically similar to the percutaneous leads, terminating in one or two long isodiametric bodies that provide connection to the stimulating electronics.įrom a stimulation selectivity standpoint, the key differences between lead types can be broken down into several categories: number of contacts, intercontact center-to-center spacing, contact length, contact width, contact shape, intraspinal lead shape, and for paddle designs with multiple columns, the relative orientation of the contacts among columns. 
Given their shape, most paddle leads must be placed via surgical procedure, such as laminotomy or laminectomy. Paddle leads, in contrast, differ in that their distal ends are relatively flat and wide, with round or rectangular plate contacts placed on one side of the flat portion, and are constructed of a flexible silicone.  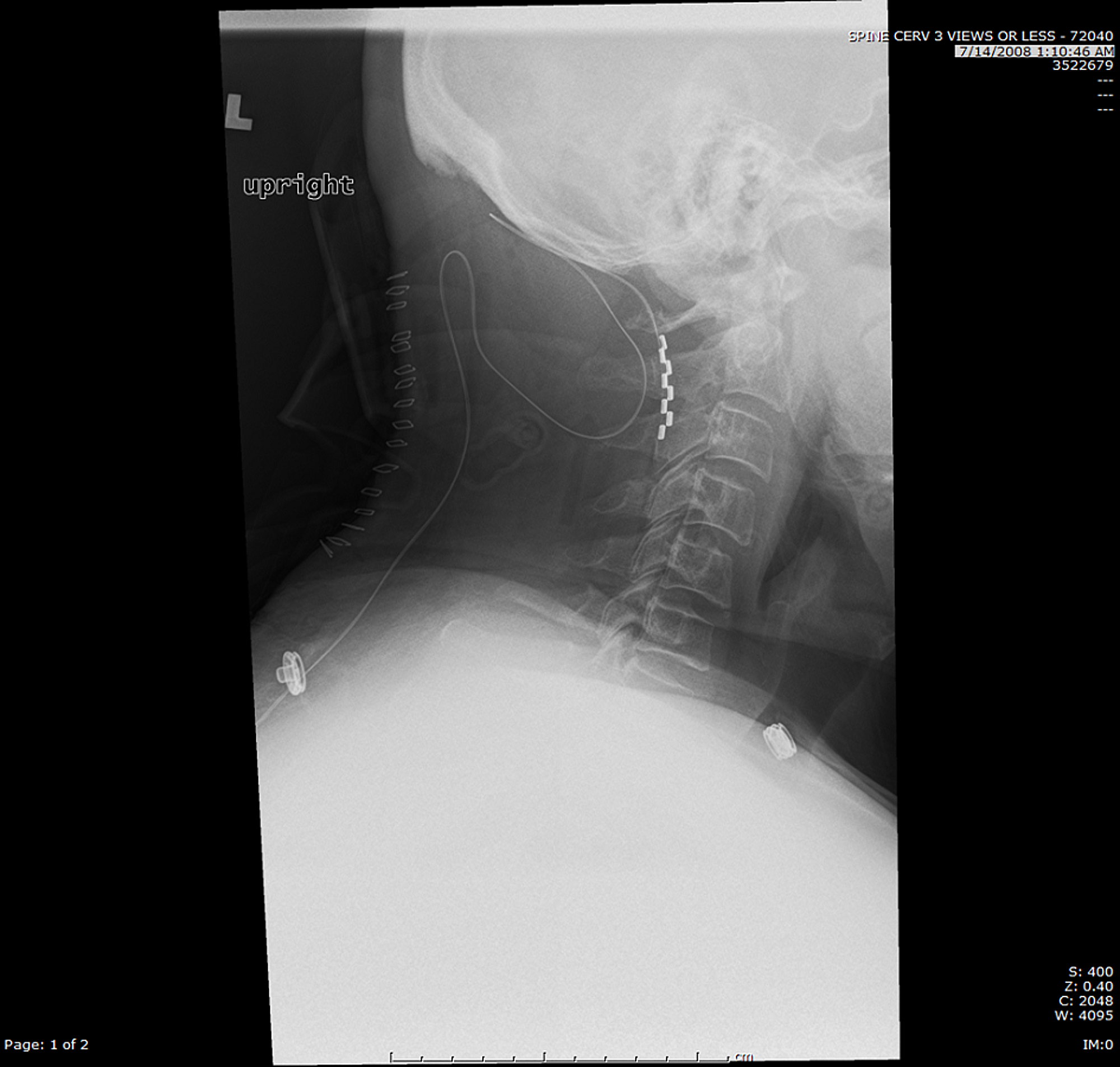
The lead itself consists of an isodiametric polyurethane body containing wires that connect the intraspinal contacts to a proximal connector, for connection to the stimulator electronics. The contacts on the leads are cylindrical, most commonly 3 mm in length, and made of platinum–iridium alloys. Briefly, percutaneous leads are catheter-like, being cylindrical and flexible, and these mechanical features allow them to be introduced into the spinal column via a spinal needle (Touhy, Husted, or the like). The main differences between the two types have been described in the literature. Two types of lead are presently in use for SCS: percutaneous and paddle. This requirement is the main driving force behind the technological developments in lead and stimulator power source design. In sum, neurostimulation differs greatly from other electrical stimulation in that it requires a high degree of stimulation selectivity. Thus, in neurostimulation, recruitment is a graded function and should be confined to the targeted nerves. This benefit is proportional to the number of targeted nerves stimulated and inversely related to the number of undesired nerves stimulated. The intent of neurostimulation is to activate only those nerves that create the therapeutic benefit. In neurostimulation applications, however, the nerves surrounding the contacts often have multiple functions (e.g., sensory, motor, autonomic), complex geometries (e.g., DRs, DCs), and differing thresholds. Also, the physiologic result of the stimulation is usually “binary.” For example, in a cardiac pacer, enough charge needs to be delivered to the endocardial stimulation site to trigger a heart contraction, and no more. In common electrical stimulation applications, such as cardiac pacing and defibrillation, there are usually no more than 1–2 stimulating contacts near the tissue to be stimulated, e.g., a bipolar pair of contacts placed in the right ventricular apex for bradycardia pacing. This article will discuss two categories of technology that enable the improvement in stimulation selectivity, the lead and the power source. Technology has accelerated in the last decade to continually improve this capability. In order to optimize this result, the SCS system, like any neurostimulation system, must provide adequate neural selectivity that is, maximal control over stimulation of the targeted nerves while avoiding stimulation of undesired neurons. 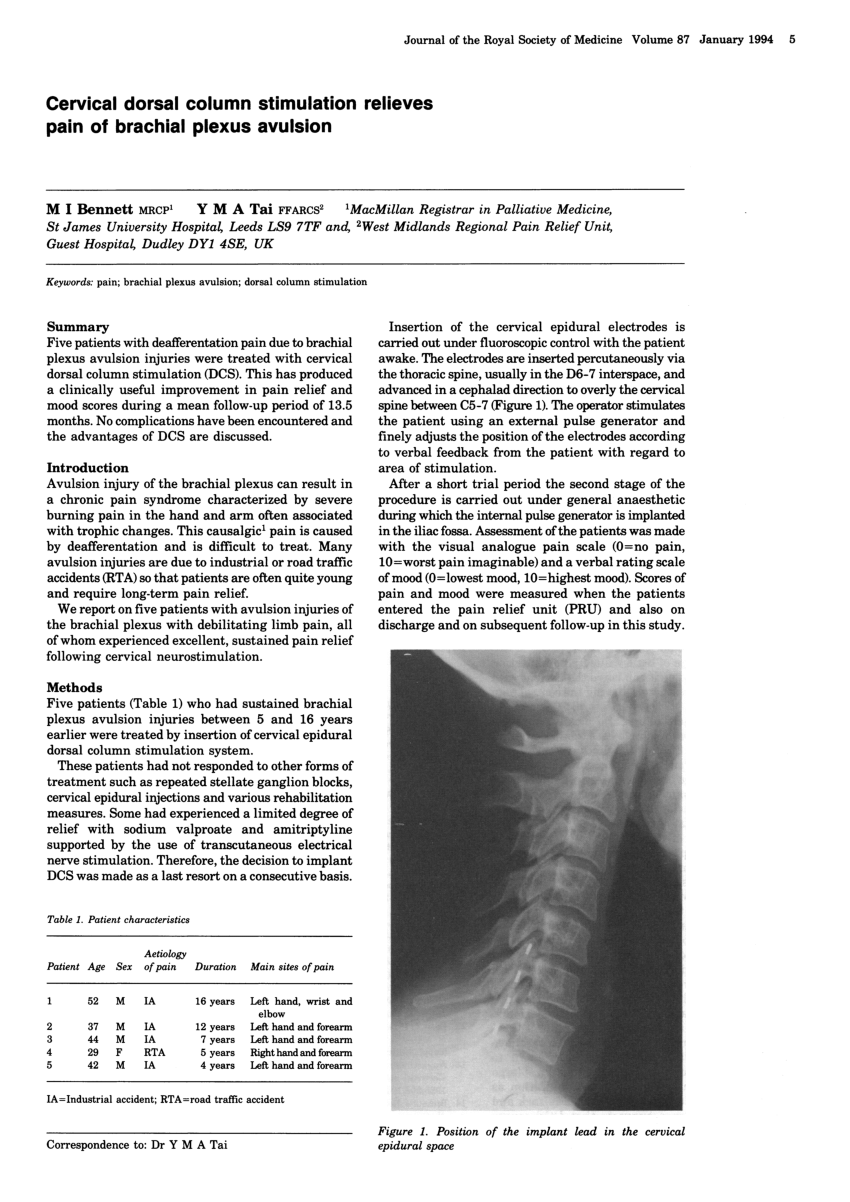
In the application of SCS, a crucial technical result that is correlated to a successful clinical outcome is the overlap of the painful areas with paresthesia. Clinically, SCS creates an epiphenomenon called paresthesia, which has been described by patients as a “tingling” sensation in their skin. Stimulation of these fibers results in inhibition of activity in the lateral spinothalamic tract (a known pain pathway), as well as increased activity in descending antinociceptive pathways. These contacts, connected to a pulse generator, are then programmed in contact combinations of anodes and cathodes, with the intent of generating an electric field, which stimulates the axons of dorsal root (DR) and dorsal column (DC) fibers in the spinal column. In SCS, an array of stimulating metal contacts is placed in the dorsal epidural space. The most successful results have been in the treatment of neuropathic pain, often with a vascular component. Spinal cord stimulation (SCS) has been used for over 30 years to treat a variety of pain conditions. Spinal Cord Stimulation, Lead, Electrode, Rechargeable Introduction 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
